December 26th, 2016 •
Comments Off on Hormonal Therapies For Adrenal Fatigue

We have already discussed a few valuable tools that can be used as part of a treatment plan in the form of nutritional supplements, herbal therapies and glandulars. In this article we will discuss a very powerful treatment tool that can be very helpful in some more severe cases of Adrenal Fatigue:
bio-identical hormone replacement for Adrenal Fatigue
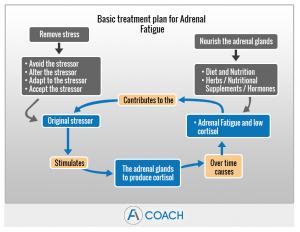
Bio-Identical Hormone Replacement Therapy
Hormones are chemical messengers that are involved in different functions and processes in your body such as development and growth, metabolism of food, reproductive health, cognitive function, mood and maintenance of body temperature. It takes only very small amounts of hormones to produce major changes in the body. Even a minor excess of hormone secretion can lead to health conditions, as can a minor deficiency in a hormone. Many hormones may become imbalanced due to stress, lack of sleep, poor lifestyle choices and a poor diet. But also due to aging many levels of hormones start to naturally decline in the body. This decrease brings with it side effects ranging from the annoying to the debilitating. Decreased sex drive, decreased bone density, sleeplessness and increased risk for osteoporosis are some of the most common complaints and concerns.
One way to maintain declining hormone levels is through hormone replacement therapy. Hormone replacement is a very powerful form of therapy wherein patients, during the course of medical treatment, receive hormones to supplement their own lack of hormones. This can be very useful as a short-term therapy, allowing your endocrine system and adrenal glands time to completely rest and recover. For most hormones you will need a prescription in the USA, but a few hormones such as DHEA and pregnenolone can be bought over-the-counter.
The Difference Between Adrenal Glandular Extracts and Hormone Replacement Therapy
Before we move on it is important to understand the difference between adrenal glandular extracts and hormones as there is often times confusion between the two. Adrenal glandular extracts nourish and help rebuild the adrenal glands, so that as the glands recover, they can once again produce the proper amount of the various hormones needed for the many functions performed by the adrenal glands. Adrenal glandulars extracts more or less correct a problem and they can be discontinued once they have done their job of repairing adrenal function. External hormones on the other hand treat the symptoms but may weaken glandular function in the process, frequently resulting in a diminished ability to resume the task of manufacturing the normal hormone levels. Many studies therefore recommend to gradually stop hormone replacement over time instead of suddenly stopping it.
So why then use hormone replacement therapy?
Bio-identical hormones are typically used to treat symptoms of perimenopause, menopause, andropause, thyroid dysfunction and Adrenal Fatigue, however other symptoms may be treated as well. When you suffer from Adrenal Fatigue at the early stages it is possible to reverse this condition by making changes in lifestyle, dietary improvements and adding in some nutritional supplements, herbal therapies or adrenal glandulars. Yet people in the more advanced stages of Adrenal Fatigue may require in some instances also hormonal supplementation in the form of hormone replacement to give the glands some much needed rest in the short-term.
Synthetic Hormones VS. Bio-Identical Hormones
Hormone replacement is somewhat still distrusted as there have been many mistakes made over the past 3 decades. Mistakes such as replacing hormones at the wrong time, replacing hormones without also replacing the balancing hormones that control hormone balance between different hormones or the use of synthetic hormones rather than bio-identical hormones.
Until recently healthcare professionals used synthetic hormones for women who experienced changes in hormone levels such as during menopause. However over the last few years studies have shown that synthetic hormones can cause women to experience and develop blood clots, stroke, breast cancer or other dangerous health conditions. Bio-identical hormones offer an effective and safe alternative to synthetic hormones and come with several health benefits. What then is the difference between synthetic hormones and bio-identical hormones? Simply said, a synthetic hormone is a hormone created in a laboratory from synthetic (man-made) chemical compounds. Bio-identical hormones are created in a laboratory from plant sources (usually soy or wild yam).
The significant difference between synthetic hormones and bio-identical hormones however, is how they act in the human body. Synthetic hormones have a chemical structure that may be similar to, but is not exactly the same as the hormones produced by the body. This means that they are not metabolized efficiently, and can, according to some researchers, release toxins into the body. Synthetic hormones may be patented (unlike bio-identical hormones) by pharmaceutical companies. As such dosage varies only slightly determined by your doctor while the molecular structure of the prescribed hormone is the same for every single person using that hormone.
Bio-identical hormones on the other hand are recognized by the human body because their chemical structure is exactly identical to the hormones produced naturally in the body. Because the chemical structure of bio-identical hormones is recognized by the human body, they are more efficiently metabolized and excreted from the body and they are not known to be carcinogenic. An extra benefit of bio-identical hormones is that each dose is tailored specifically to the needs of the individual, not simply what dose the pharmaceutical company offers as is the case with synthetic hormones.
Studies Show Bio-Identical Hormones Are Safer…..
Many European studies show that bio-identical hormones are safer than synthetic hormones. In fact, there is ample evidence that suggests that certain bio-identical hormones even have an anti-cancer effect (). However, that doesn’t mean that bio-identical hormones are perfect as most research is relatively new and even bio-identical hormones do not come without side effects. DHEA for instance easily converts into testosterone which may be problematic especially for women (). While administering cortisol may prevent the adrenal glands from producing cortisol themselves (). Hormone replacement therapy should always be monitored by a doctor or specialist experienced in the use of hormone therapy.
Before we move on to discuss each individual hormone, here are a few aspects of hormone replacement that you need to be aware of:
- Hormone replacement is a very powerful tool for treating Adrenal Fatigue and you should see this as sort of a last resort. So before you consider hormone replacement make sure you have made changes to your dietary plan and lifestyle first.
- Every person has different hormonal needs, so treatment needs to be personally tailored.
- When you begin hormone replacement, your healthcare practitioner should determine your baseline hormone levels and keep following your hormone levels during treatment to see whether your dosing needs to be adjusted periodically.
- Supplementing one hormone can affect the levels of other hormones, so be aware of possible side effects. Supplementing DHEA for example may alter the levels of testosterone and/or estradiol in some people.
- Even though your hormonal profile may suggest that hormone replacement is necessary, your personal health situation may prevent the use of hormone replacement. For example, a personal family history of breast, ovarian, or endometrial cancer and a strong family history of breast or ovarian cancer makes hormone replacement possibly inadvisable.
In summary, hormone replacement can be a powerful recovery tool to those suffering from Adrenal Fatigue. However, even bio-identical hormones do not come without side effects and they need to be used only under the supervision of a skilled doctor or specialist. Generally, bio-identical hormone replacement should be used as a last resort, only after you have made the necessary changes to your dietary plan and lifestyle.
Bio-identical Cortisol
In general, cortisol treatment should be considered as a last resort in the more severe cases of Adrenal Fatigue and then only as a temporary measure allowing the adrenal glands time to completely rest, thereby providing an opportunity for them to recover. If your activities of daily life are affected and changes in your diet, lifestyle and nutritional interventions have not produced significant results, it could be worth discussing this option with your doctor. In most other cases of Adrenal Fatigue the use of bio-identical cortisol may actually work counterproductive. Firstly, this is because the use of replacement cortisol can lead to a host of side effects and secondly cortisol replacement stops (or significantly slows down) the body’s own production of cortisol (while in fact you want to stimulate the body’s own production of cortisol) ().
Cortisol is typically only available by prescription and treatment should be monitored by a doctor experienced in treating Adrenal Fatigue using bio-identical hormones. Bio-identical cortisol is commonly known under the names of Hydrocortisone or Cortef. Typically a total divided dose of under 20 mg per day is considered a very safe dose by most doctors and should not produce negative side-effects. That said, there is no uniform prescribing standard as treatment should be individually tailored. After you have been taking cortisol replacement you should taper off of the therapy slowly, to allow your adrenal glands time to ease back into production again. The longer you have been using replacement hormones, the longer the weaning process needs to last.
DHEA
DHEA or Dehydroepiandrosterone is a steroid hormone created from pregnenolone (which itself is metabolized from cholesterol) by the adrenal glands, testes in men or ovaries in women and the brain. Research has shown that low DHEA levels are a general marker for many degenerative diseases, accelerated aging and this hormone plays an important factor in a host of health problems such as chronic fatigue syndrome and stress disorders. DHEA levels usually peak when we’re in our mid-20s and decrease with age. By the time we reach 40 our bodies create about half as much DHEA as it used to. By the mid-60s, DHEA has dropped to 10-20% of its peak value. This natural decline is often aggravated with chronic stress, which in the course of time may result to Adrenal Fatigue and hormone dysfunction.
The recommended daily dose range is 5-25 mg for women, 25-75 mg for men. The initial dose is determined by gender and baseline DHEA level (the lower the level, the higher the starting dose) (). DHEA is not controlled by a feedback loop system that shuts off production when levels get high. So taking supplements of DHEA won’t suppress your body’s production of this hormone. However just like with any other hormone replacement therapy DHEA replacement too should be conducted under the supervision of an experienced doctor.
Several studies lasting anywhere between six months and a year at doses varying from 25 to 200 mg per day have shown DHEA to be safe with minimal side effects. The biggest concern over DHEA supplementation is the conversion of DHEA into either androgens (testosterone, dihydrotestosterone, androstenedione) or estrogens (estrone, estradiol). A significant androgen increase in women may lead to acne, deeper voice and facial hair growth, while in men a decreased testosterone level coupled with an increase in estradiol may lead to irritability, insomnia, fatigue and development of breast tissue. With the right dosing DHEA has been found to be safe and almost totally without risk of side effects, particularly when your hormone levels are checked regularly and you are under a doctor’s supervision.
Pregnenolone
Pregnenolone is called the “mother hormone” because it is used by the body to create all other steroid hormones through the hormone synthesis pathway. As such this may be one of the most important hormones, because as a precursor to many other hormones it can bring the levels of other hormones up or down as needed. Pregnenolone replacement is linked to improvements in many symptomatic troubles for those with Adrenal Fatigue such as increasing resistance to stress, improving physical and mental energy, enhancing nerve transmission and memory, reducing pain and inflammation and reducing symptoms of PMS and menopause.
A typical recommended dosage of pregnenolone is 15-100 mg to be taken daily, preferably in the morning or at midday (). As with any supplement, you should take pregnenolone in the dose your doctor determines is beneficial for your individual circumstances.
Testosterone
Testosterone is made in the testicles and ovaries, in smaller amounts by the adrenal glands and is also found in brain tissue. Although it is thought of as a “male hormone” it also plays an important role in women. Both men and women (men produce about 10 times the level of women) produce and use testosterone and their testosterone levels peak during youth and decline with age. Symptoms of low testosterone include erectile dysfunction in men as the most common symptom. There are several other symptoms that can occur in both men and women (for example, low sex drive, fatigue, bone and muscle tissue loss, depression).
Dosing for women usually starts off with 0.5 mg per day and women often find their best dose to be around 2.5mg per day. Men’s doses are typically much higher ranging from 20 mg to 100 mg per day. If you and your doctor decide that you need treatment, there are several options for bio-identical testosterone replacement. Testosterone products and supplements come in many forms including transdermal gels, oral lozenges, implantable pellets and injectable testosterone. Factors such as insurance coverage, cost, ease of administration, convenience and potential side effects all play a role when deciding on the best available replacement option.
Progesterone
Progesterone is a hormone that is found in much higher concentrations in women than in men. It is secreted primarily by the ovaries in females and by the testes in men. Smaller amounts are produced by the adrenal glands and in the brain cells of both women and men. Progesterone is a precursor to cortisol and other important steroid hormones. If progesterone levels decline, so can these other hormones, which have their own important roles in our physiological health.
Progesterone plays a large role in the body performing important functions in both males and females of all ages. Progesterone is responsible for regulating blood sugar, bone building, protection against osteoporosis and developing intelligence. Additionally, progesterone promotes fat burning for energy, regulates thyroid hormone production, and helps maintain sex drive. It also acts as a natural antidepressant, aids in normalizing blood clotting, improves premenstrual symptoms (PMS) and normalizes zinc and copper levels along with many other vital functions.
When women reach the age of 35-40, levels of progesterone and estrogen begin to decline. From this period up to age 50, there is a 35% drop in estrogen and a 75% reduction in progesterone (). As a consequence many premenopausal and menopausal are overloaded with estrogen and suffer from a progesterone deficiency. There is then not enough progesterone to counteract the amount of estrogen in the body. This imbalance between estrogen in relation to progesterone is referred to as “estrogen dominance” and can result in symptoms of PMS, perimenopause, or menopause.
Bio-identical progesterone may come in several forms such as topical creams, troches (dissolved in the mouth) or oral capsules. Each of these have their advantages and disadvantages. It’s important to discuss these with your qualified healthcare professional so that you choose the safest and most effective option. The typical dose for women may vary between 25-100 mg, depending upon a woman’s individual biochemical needs. Men rarely supplement progesterone.
Estrogen
While estrogen is considered to be primarily a female hormone, estrogen plays an important role in men too. In women, estrogen is created mainly in the ovaries, but it is also created by fat cells and the adrenal glands. Estrogen actually has several different subforms such as; estrone (E1), estradiol (E2) and estriol (E3). Typically when one is talking about estrogen, they refer to estradiol (E2).
Estrogen levels fall after menopause, or when a woman stops menstruating. This reduction in estrogen production can lead to a host of symptoms such as hot flashes, vaginal dryness and loss of sex drive. Estrogen levels don’t plummet as much as progesterone, in fact far more women have too much estrogen relative to progesterone as discussed in the progesterone section ().
Just like women need small amounts of testosterone, men need small amounts of estrogen too. In men estrogen is actually made from testosterone by a special enzyme called aromatase. As men age, they tend to make higher levels of estrogen with lowered production of testosterone. High estrogen levels in men contribute to prostate cancer and heart disease as well as gynecomastia. Excessive levels of estrogen in men are correctible and reversible by balancing hormones, proper diet and lifestyle changes.
The compounded estrogen formulations most frequently prescribed to women contain 2 or 3 forms of estrogen in varying percentages. Two popular formulations are BiEst (80% estriol and 20% estradiol) and TriEst (80% estriol, 10% estradiol and 10% estrone). They are generally available in oral and transdermal preparations. TriEst is not often used anymore nowadays due to concerns with estrone (E1) content. A common starting point of BiEst is 1mg per day, sometimes divided into two doses (.5 mg per dose) building up to 2.5 – 5 mg daily.
References & Further Reading